
You know that sinking feeling when the “Check Engine” light pops on in your car? You don’t know what’s wrong, but you know it’s going to be expensive, and you’re at the mercy of the mechanic. You trust them because, well, they have the tools and you don’t.
Now, imagine that feeling, but instead of a sedan, it’s your body. And instead of a mechanic, it’s a surgeon in a white coat telling you that you have a “blockage” or “degeneration.” It’s terrifying. You nod, you sign the forms, and you schedule the surgery because you’re scared.
But here is the hard truth that most people don’t talk about: Just because a mechanic recommends a new transmission doesn’t mean the car won’t run fine without it.
In the American medical system, we are currently facing an epidemic of what experts call “low-value care.” That’s a polite way of saying “medical treatments that cost a fortune, hurt a lot, and don’t actually make you healthier.” For those of us over 50, this is a massive issue. We are being sold repairs for standard wear-and-tear that our bodies might not actually need.
I’ve dug through piles of Medicare claims data, audit reports, and peer-reviewed studies to bring you this list. These aren’t fringe theories; this is based on data from the Office of Inspector General (OIG) and the Lown Institute. We’re going to look at eight specific procedures that are routinely over-scheduled, why they happen, and—most importantly—how you can look a doctor in the eye and legally, safely say, “No thanks.”
1. The “Medicare Auditor” — The Accidental Whistleblower

So, who exposed this? It wasn’t a doctor with a guilty conscience. It was the accountants.
Meet the Medicare Auditor. These are the folks tasked with protecting the Medicare Trust Fund. Their job is to hunt for “improper payments.” They look at claims and ask, “Was this medically necessary?”.
When they audit a hospital, they aren’t looking for bad medical advice; they’re looking for waste. But in the process, they inadvertently shine a spotlight on a massive open secret: doctors do a lot of stuff that isn’t necessary.
For example, auditors recently found that hospitals were billing millions for “spinal fusions” that didn’t meet the criteria for coverage. They weren’t fraud in the sense of a fake surgery; they were real surgeries that the data says shouldn’t have happened. The OIG releases a “Work Plan” every year that basically lists the procedures they are suspicious of—it’s like a roadmap of medical overuse.
Why does this happen? Is your doctor trying to hurt you? No. But the system is designed to pay for action, not inaction. A hospital gets paid to fill beds. A surgeon gets paid to cut. There is no billing code for “sat down with the patient for an hour and explained why they should just go for a walk.”
The “Clogged Pipe” Myth
The Plumbing Model
The Myth: Your arteries are like pipes. If one is 90% clogged, common sense says you must “roto-rooter” the drain.
It is intuitive. It makes sense. It is also WRONG.
The Data Shock
During the COVID-19 pandemic, doctors performed over 45,000 stents on patients who were actually stable.
Even prestigious hospitals had overuse rates double the national average.
Why It’s Unnecessary
Heart attacks aren’t usually caused by big, hard, calcified blockages. They are caused by the rupture of smaller, soft, “vulnerable” plaques you can’t even feel.
The Evidence
Huge trials like COURAGE, ISCHEMIA, and ORBITA have spoken.
Let’s start with the big one. If I told you that your heart arteries are like plumbing pipes, and one is 90% clogged, common sense says you have to roto-rooter that drain, right?
That is the “Plumbing Model” of heart disease. It makes perfect sense. It’s intuitive. It’s also wrong.
The Data Shock
During the first year of the COVID-19 pandemic—when hospitals were supposed to be saving beds for emergencies—doctors performed over 45,000 coronary stents on patients with stable heart disease. That’s one in five stents that, according to the data, didn’t need to happen.
Major hospitals—we’re talking prestigious places like the Cleveland Clinic and Mt. Sinai—had overuse rates double the national average.
Why It’s Unnecessary
Here is the science part, but I’ll keep it simple. Heart attacks aren’t usually caused by those big, hard, calcified blockages that cause chest pain (angina). They are caused by the rupture of smaller, soft, “vulnerable” plaques that you can’t even feel.
When you stent the big blockage, you fix the pain, but you don’t stop the heart attack. The other plaques are still there, waiting.
- The Evidence: Huge trials like COURAGE, ISCHEMIA, and ORBITA proved that for stable patients, stents do not prevent heart attacks or extend life any better than medication and lifestyle changes.
3. Spinal Fusion (The “Grey Hair” of the Spine)
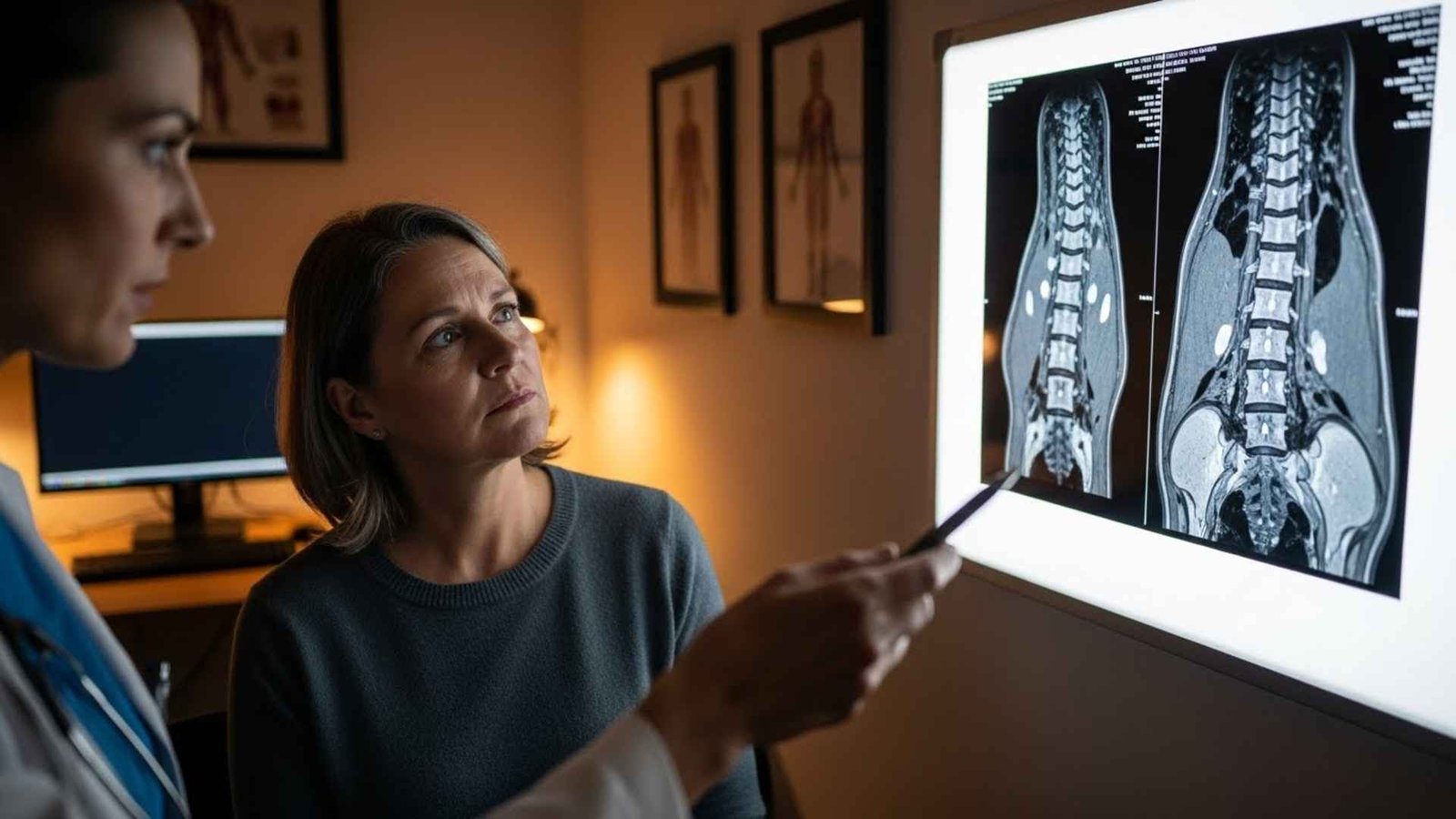
If you are over 50 and you get an MRI of your back, it’s going to show “Degenerative Disc Disease.” That sounds horrifying, like your spine is crumbling.
But here’s the thing: That is normal. It’s like having grey hair, but on the inside.
The $2 Billion Mistake
Surgeons often look at that MRI and suggest a Spinal Fusion—welding vertebrae together to stop the pain. But the Lown Institute found that we wasted about $2 billion on unnecessary back surgeries over just three years.
The Trap
When you fuse the spine, you stop movement in that spot. Physics dictates that the stress has to go somewhere else. It goes to the discs above and below the fusion. This causes Adjacent Segment Disease, which means… you guessed it, more surgery later.
Myths vs. Facts:
- Myth: “I need surgery because I have a ‘bad disc’.”
- Fact: Most back pain resolves on its own or with physical therapy. Surgery should be the absolute last resort, not the first.
4. The “Cement” Fix (Vertebroplasty)
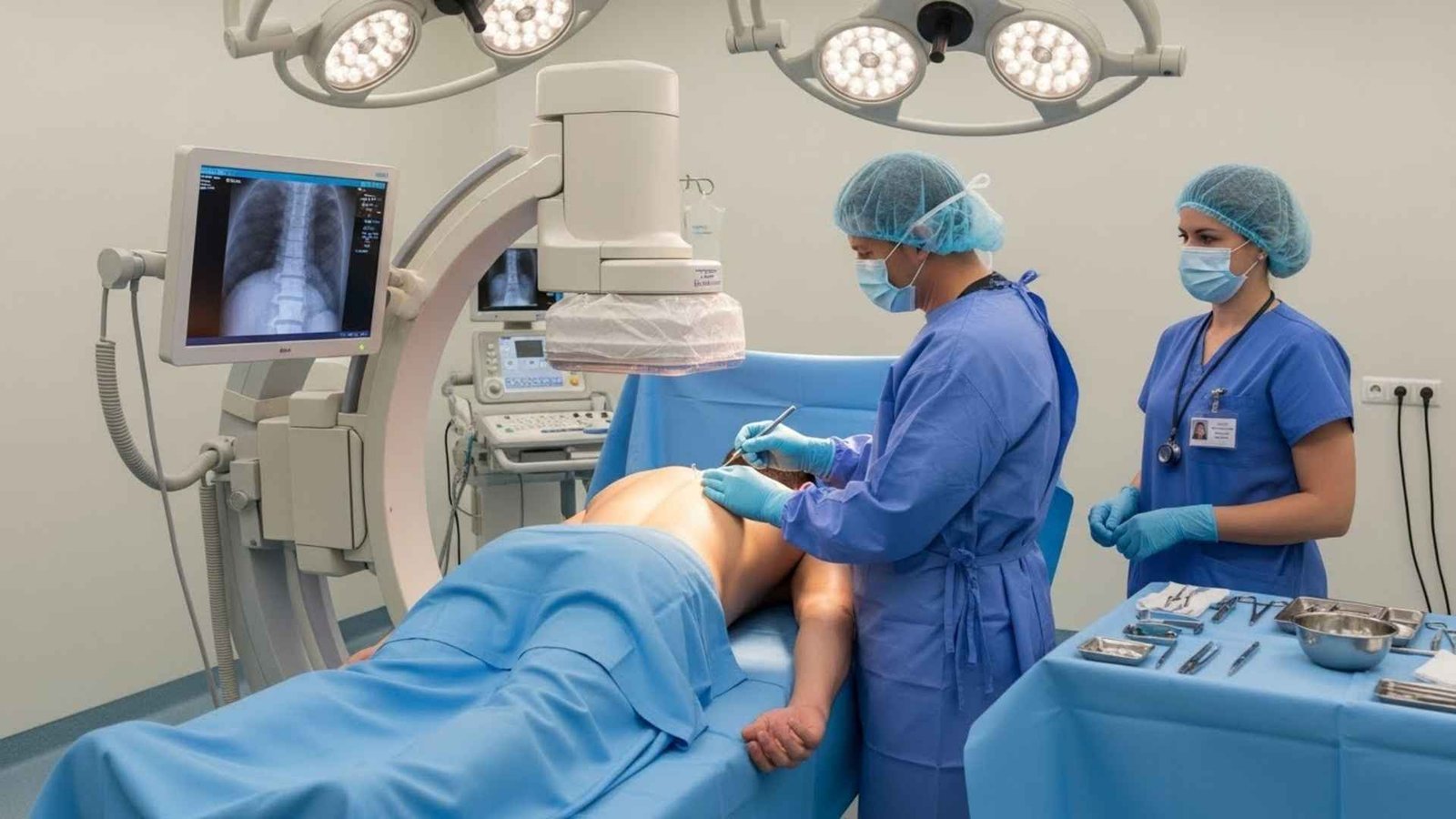
This one drives researchers crazy because it’s a “zombie” procedure—it just won’t die.
The Procedure: Older women with osteoporosis often get compression fractures in their spine. It hurts. So, doctors inject medical-grade cement into the bone to stabilize it.
The Reality: Two major studies published in the New England Journal of Medicine compared this to a “sham” procedure. They literally pretended to do the surgery on half the patients (tapped on the back, made noises, but no cement). The result? The patients who got the fake surgery felt just as much pain relief as the ones who got the cement.
Why? Because bones heal on their own, and the placebo effect is powerful. Yet, we still did over 16,000 of these in 2020 alone.
5. The Knee Clean-Up (Arthroscopy)
You’ve probably heard a friend say, “I’m just going in to get my knee cleaned out.” They mean arthroscopy—using a tiny camera to trim torn cartilage (meniscus).
If you are a 25-year-old athlete who blew out your knee on the field? Great surgery. If you are 60 and your knee clicks when you walk? It’s probably useless.
The Placebo Effect in Action
For degenerative knees (arthritis), this surgery works about as well as physical therapy, but with surgical risks. In fact, studies show that after 6 to 12 months, there is zero difference in pain or function between people who got surgery and people who just did exercise.
We are seeing a drop in these surgeries (down 74% in places like Finland), but in the U.S., it’s still a cash cow.
6. Hysterectomy (The “Castration” Controversy)

Ladies, this one is tough to talk about, but we have to. Hysterectomy (removing the uterus) is the second most common surgery for women. And while it saves lives when it comes to cancer, it is massively overused for benign things like fibroids.
The “Castration” Issue: Often, surgeons will take the ovaries out “while they’re in there,” just to prevent ovarian cancer. They call it “prophylactic.” But removing the ovaries before age 65 significantly increases your risk of heart disease, osteoporosis, and cognitive decline. You are trading a small risk of cancer for a huge risk of everything else.
The Alternative: There are so many other options now! Uterine Artery Embolization (UAE) shrinks fibroids without surgery. Don’t let anyone tell you the only solution is to “take it all out” without a second opinion.
7. The Stroke Risk Paradox (Carotid Endarterectomy)
This is a surgery to scrape plaque out of the arteries in your neck to prevent a stroke.
Here is the paradox: The surgery itself carries a risk of causing a stroke (about 3%). If you have no symptoms (you feel fine, but the doctor heard a “whoosh” sound), your annual risk of having a stroke from that plaque is now very low—about 0.5% to 1%—thanks to modern meds like statins.
Do the math: Why take a 3% risk of a stroke today to prevent a 1% risk of a stroke next year? For asymptomatic patients, the math just doesn’t add up anymore.
The “Spider” Trap
1. The Trap
It’s a little metal spider trap placed in your main vein to catch blood clots.
2. The Glitch
These things are meant to be TEMPORARY.
The problem? We forget to take them out. Thousands of patients still have them left inside.
3. The Fallout
When left inside, they can:
- Migrate ✈️
- Puncture the vein 💉
- Actually CAUSE more clots 🩸
📉 Retrieval rates: Shockingly Low.
An IVC filter is a little metal spider trap they put in your main vein to catch blood clots. It sounds like a great safety net.
The problem? We forget to take them out. These things are meant to be temporary. But thousands of patients have them left inside, where they can migrate, puncture the vein, or actually cause more clots. The FDA has issued warnings, yet retrieval rates are still shockingly low.
Need More Help For Managing Pain at Home? Look Into These
Sometimes, the best way to avoid a surgical procedure is to manage the symptoms effectively enough that you no longer feel desperate for a “fix.” While no product replaces a good doctor, having the right tools at home can give you the relief—and the data—you need to delay invasive interventions confidently. Based on the topics we covered, here are a few highly-rated items that might help you stay in the driver’s seat of your own health.
1. Back Mechanic by Dr. Stuart McGill

If you have back pain, this is often considered the “Bible” of non-surgical recovery. Dr. McGill is a world-renowned spine expert who guides you through self-diagnosing your specific pain triggers and “tuning” your back to avoid surgery. It’s a must-read before you sign up for fusion.
2. Omron Platinum Blood Pressure Monitor

Before you get on the “cascade of care” for heart issues, you need accurate data. White coat syndrome (high BP only at the doctor’s office) is real. This monitor is known for high accuracy and can even detect AFib, helping you and your doctor make better decisions based on home trends, not just one stressful office visit.
3. Everlasting Comfort Lumbar Support Pillow

Postural stress is a huge driver of the “degenerative” back pain that leads to unnecessary surgery. This memory foam cushion is a simple, low-tech way to correct your posture in the car or office chair, potentially reducing the daily strain that causes flare-ups.
4. TENS 7000 Digital TENS Unit

Instead of jumping to injections or surgery for knee or back pain, many physical therapists recommend TENS (Transcutaneous Electrical Nerve Stimulation). This prescription-strength unit interrupts pain signals to the brain, offering drug-free relief that might just get you through a flare-up without a scalpel.
5. Medical Appointment Planner & Journal

“Informed Refusal” requires you to remember what the doctor said, what the risks were, and what questions you asked. A dedicated medical planner (like the ones from Clever Fox) helps you track symptoms, organize questions before the visit, and document the answers, so you aren’t swayed by pressure or anxiety in the moment.






